Bilateral Intertrochanteric Proximal Femur Fractures After Low Energy Trauma: Case Report
Moh’dKheir Aolymate1, Majdala Al-bataineh2, Abdullah Alkhawaldah1, Bashar Al Khawaled1, Zaydoun Alkhrissat1, Malek Abu Hazim1, Mohamad Elfawair1, Raed Alhnaity1, Laith Al Hseinat1*
1Department of Orthopedics, Royal Medical Services, Amman 11855, Jordan
2Faculty of Medicine, Yarmouk University, Irbid, Jordan
*Corresponding Author: Laith Al Hseinat, Department of Orthopedics, Royal Medical Services, Amman 11855, Jordan.
Received: 11 April 2026; Accepted: 13 April 2026; Published: 20 April 2026
Article Information
Citation: Moh’dKheir Aolymate, Majdala Al-bataineh, Abdullah Alkhawaldah, Bashar Al Khawaled, Zaydoun Alkhrissat, Malek Abu Hazim, Mohamad Elfawair, Raed Alhnaity, Laith Al Hseinat. Bilateral Intertrochanteric Proximal Femur Fractures After Low Energy Trauma: Case Report. Journal of Orthopedics and Sports Medicine. 8 (2026): 154-159.
View / Download Pdf Share at FacebookAbstract
Introduction: Hip fractures are significant global health concern, due to high morbidity and mortality especially for elderly patients. Simultaneous bilateral intertrochanteric fractures are rare injuries typically linked to high- energy trauma, but they can also happen to osteoporotic patients following low-energy mechanisms.
Case Presentation: We report a rare case of simultaneous bilateral intertrochanteric femur fractures due to low-energy trauma in an elder patient who was presented to our tertiary Hospital Emergency department (King Hussein Medical Hospital). The patient received surgical treatment using closed reduction internal fixation methods specific to each fracture pattern. To maximize healing after surgery, early mobilization and multidisciplinary care were used. During follow-up, the patient showed good functional improvement and no significant complications.
Discussion/Conclusion: Simultaneous bilateral intertrochanteric fractures provide considerable therapeutic challenges due to their rarity, complexity, and increased physiological strains on the patients involved. In low-energy trauma, osteoporosis is a major factor in pathogenesis. Stable fixation that permits early mobilization is essential for functional recovery and may reduce postoperative complications and opioid dependence which should be among the goals of surgical management and hence enhance results. This case emphasizes the significance of customized surgical planning, early rehabilitation, and a multidisciplinary approach.
Keywords
Bilateral intertrochanteric fractures; Hip fractures; Osteoporosis; Elderly patients; Low-energy trauma; Intramedullary fixation; Early mobilization; Rehabilitation; Surgical management
Article Details
1. Introduction
Proximal femur fractures continue to be a significant healthcare problem and a major consequence in elderly. According to epidemiological data, these fractures still cause a substantial clinical and financial burden. Due mostly to population ageing, declining bone mass, and an increased risk of falls. The incidence is predicted to increase globally, reaching up to 21.3 million cases by 2050 [1,2]. Falls, osteoporosis, and trauma are frequently linked to proximal femur fractures, which are among the most frequent fractures, especially in older people [3]. The most frequent mechanism of injury among elder patients is low-energy falls, especially from standing height [4]. The incidence is impacted by age, sex, comorbidities, and lifestyle among people 65 and older, which differs throughout nations; it is more prevalent in women, especially those with cognitive impairment and institutionalization, and peaks in patients between the ages of 85 and 89 [1].
Apart from the immediate consequences, individuals who sustain proximal femoral fractures are susceptible to other insufficiency fractures, especially those involving the contralateral femur, with reported rates ranging from 2.1% to 15%, and these incidents are linked to a higher mortality rates and further functional deterioration [5]. An increased risk of subsequent contralateral fractures, especially within the first two years, is also linked to a history of prior fractures, particularly hip fractures [4]. Since only 40–60% of older patients restore their pre-fracture level of mobility and independence within a year, these fractures frequently represent a life-altering event, and many of the affected patients are weak or on pre-existing care [6]. Reduced bone strength is closely linked to osteoporotic hip fractures, which are a major cause of disability and death in older individuals, and many patients are unable to return to their pre-injury level of independence as a result [7].
The majority of femur fractures are hip fractures, which are typically divided into three categories: subtrochanteric, intertrochanteric, and femoral head/neck fractures [8]. Intertrochanteric and subtrochanteric fractures are among the intracapsular and extracapsular kinds of proximal femur fractures [6]. Treatment usually entails surgery; femoral neck fractures in elderly patients are frequently treated with arthroplasty, whereas intertrochanteric and subtrochanteric fractures are primarily treated with intramedullary implants for internal fixation, with intramedullary nailing being a common approach to allow early mobilization and weight bearing [3,9]. Even with improvements in care, problems like infection and poor fracture healing still exist [3].
Femoral neck, intertrochanteric, and subtrochanteric fractures seem to have similar short-term mortality and overall complication rates, but there are notable differences in certain postoperative patterns. Because of their metaphyseal location, greater vascular supply, and use of intramedullary implants, intertrochanteric and subtrochanteric fractures are linked to increased rates of postoperative blood transfusion. In contrast, femoral neck fractures exhibit greater rates of reoperation and readmission, perhaps due to complications from arthroplasty or fixation failure, while intertrochanteric fractures typically have lower failure rates because of intact blood flow [10].
In clinical practice, fracture classification is crucial because it offers a standardized communication system, directs treatment choices, and forecasts prognosis. The AO/OTA categorization system, which is frequently used for proximal femur fractures, has undergone multiple updates, and advances in imaging modalities, especially computed tomography (CT) and three-dimensional reconstruction (3D-CT), have improved the understanding of fracture patterns and supported the development of classification systems [11].
In a clinical setting, hip fractures usually manifest as pain, inability to bear weight, and characteristic deformities such as external rotation and limb shortening [4]. Elderly hip fractures are usually the result of low-energy falls and are impacted by multiple factors including osteoporosis, weakened muscles, and poor balance [7].
We aim to report a rare case of bilateral intertrochanteric proximal femur fractures in an elderly adult after low energy trauma. The patient was presented atypically because classical deformities was absent.
2. Case Presentation
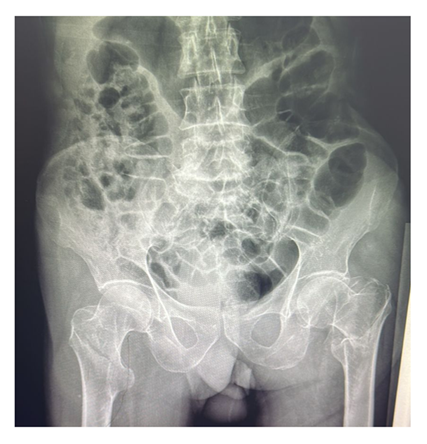
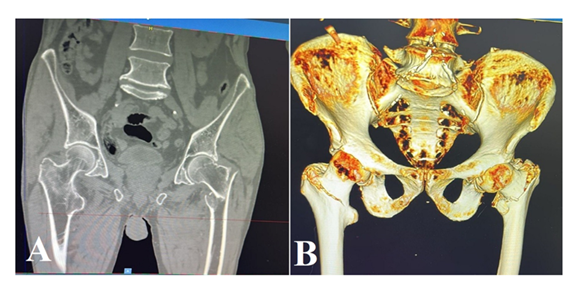
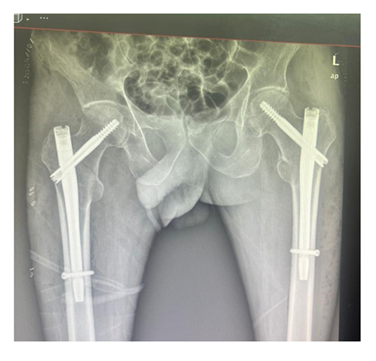
A 69-year-old male was presented to the emergency department complaining of hip pain with inability to bear weight due to falling down from his standing position 2 hours prior to his administration, the physical examination showed he was conscious, alert, afebrile, with stable vital sign, the pain severity was 8/10 on presentation and the bilateral hip pain was associated with limited ROM, log roll positive, no shortening nor external rotation deformity in both hips, distal pulses were intact, and absence of neurological deficits was confirmed. Laboratory investigations revealed leukocytosis (WBC 14.8 ×109/L), elevated C-reactive protein (7.71 mg/L), and thrombocytosis (platelets 681 × 109/L). Hemoglobin was 12.6 g/dL with a hematocrit of 37.8%. Renal function tests were within normal ranges (creatinine 0.87 mg/dL, urea 17.9 mg/dL). Electrolytes levels were normal (sodium 142.2 mmol/L, potassium 4.31 mmol/L). Random blood sugar was 142 mg/dL. INR was 1.01. The patient denied any red flag symptoms, including weight loss, unintentionally, over the past year. Given the clinical presentation, radiographic evaluation was performed and revealed bilateral intertrochanteric fractures of the proximal femur (Figure 1) CT was done for further assessment and Preoperative evaluation (Figures 2). Accordingly, the patient was admitted for surgical fixation. upon admission, Intravenous fluids with potassium supplementation, morphine sulphate (5 mg IV every 6 hours), omeprazole 20 mg, intravenous paracetamol (1 g every 8 hours), and thromboprophylaxis with low molecular weight heparin were initiated. Two units of packed red blood cells were prepared prior to surgery, and the patient was kept nil per os (NPO) after midnight. Preoperative echocardiogram showed no pericardial effusion, trace mitral and tricuspid regurgitation, intact left ventricular systolic function, and arrhythmia with paradoxical septal wall motion. After that, the patient received continuous spinal anesthesia while undergoing bilateral intertrochanteric fracture fixation utilizing short intramedullary nails. Under fluoroscopic guidance, the Surgical treatment took 2 hours and 45 minutes to complete without any difficulties and Postoperative x rays were obtained (Figure 3).
Next day after surgery the patient received physiotherapy care plan which included range of motion exercises and weight bearing as tolerated and medications included morphine sulfate (8 mg every 6 hours), omeprazole 20 mg, intravenous cefazolin (1 g every 8 hours), Revanin tab (1g every 8 hours) intravenous fluids (normal saline) 1500iu, and thromboprophylaxis with low molecular weight heparin 4500iu every 24hours.
Follow-up laboratory investigations showed packed cell volume 31.1%, leukocytosis (WBC 12.2 ×109/L), and persistent thrombocytosis (platelets 636 × 109/L), with normal renal function tests.
The patient resumed physiotherapy and pain control on the third postoperative day.
The patient was discharged by the fourth postoperative day after wound dressing. packed cell volume was 29.7%, WBC was 12.4 ×10³/L, and platelets were 612 × 10¹/L according to laboratory results upon discharge.
After two weeks, the patient was seen in the outpatient clinic for wound care and ambulation evaluation. He was using a walker for ambulation and bearing all his weight.
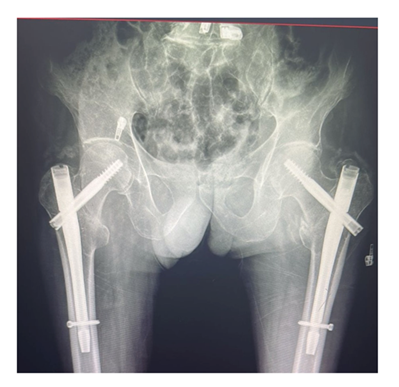
Six weeks after surgery, the patient was still clinically stable and was utilizing a walker to walk with full weight bearing. There were no documented postoperative problems, and the surgical wounds were clean and follow up radiographs were done (Figure 4). In the next follow up 3 months after surgery the patient presented to the clinic ambulating without walker in a full weight bearing manner (Figure 5).
3. Discussion
Hip fractures are a serious global public health concern, especially for the elderly. Because of the increased morbidity and mortality associated with simultaneous bilateral hip fractures. Symmetric fracture patterns, which are often treated similarly on both sides, characterize most reported cases. Asymmetrical or dissimilar fractures are less frequent and require individualized surgical techniques [12].
When compared to unilateral fractures, which are frequently observed in the elderly and may result from minor trauma, bilateral trochanteric fractures are extremely uncommon injuries. Bilateral fractures are typically linked to a more severe or complex trauma; however, they can sometimes happen in osteoporotic patients even after minor trauma. Osteoporosis is a major contributing factor to these fractures because ageing bones lose their ability to respond elastically, making them more vulnerable to damage [13].
Unlike unilateral fractures, which are much more prevalent, simultaneous bilateral intertrochanteric fractures are occurring less frequently than 0.3% of the general population. These fractures usually follow high-energy trauma in individuals with normal bone, where both lower limbs are simultaneously subjected to compressive and rotational stresses, or in circumstances like run-over accidents, crush injuries, or entrapment. However, due to decreased elastic resistance, even a small amount of force may be enough to cause such fractures in patients with inadequate bone quality, such as osteoporosis, osteomalacia, or neoplastic diseases [14].
All things considered, low-energy trauma frequently results in unilateral hip fractures in the elderly, but in extremely rare instances, it can produce simultaneous bilateral hip fractures [15].
Osteoporotic fractures frequently occur in regions with poor bone mineral density, especially around the femoral neck and intertrochanteric regions. These fractures are becoming more common as people age, which is indicative of the gradual deterioration of bone quality. Since some implants may be needed to treat several fracture sites at once, the choice of fixing technique should be customized, particularly in situations with other femoral pathologies [16].
Intertrochanteric fractures are more significantly linked to advanced age and poor overall health; femoral neck fractures are more strongly linked to low bone mineral density and poor functional ability. Furthermore, it has been demonstrated that the form of fracture affects recovery and death; intertrochanteric fractures are linked to greater short-term mortality rates than femoral neck fractures [17].
During management, choosing a surgical technique whether fixation or replacement that permits early mobilization and weight bearing is crucial when both lower extremities are affected and the fracture pattern and stability determines the best course of action. Intramedullary nails, sliding hip screws, plates, and prosthetic replacements are among the several surgical possibilities. In cases of unstable extracapsular intertrochanteric fractures, intramedullary implants are especially recommended because they offer stable fixation, reduce soft tissue injury, and improve functional results [13].
Intramedullary nails, trochanteric femoral nails, proximal femoral nail anti-rotation, dynamic hip screws, and angle blade plates are among the fixing methods that can be used, depending on the stability and configuration of the fracture. Dynamic hip screws are frequently used to treat stable fractures, while intramedullary implants are used to treat unstable fractures or those with loss of medial support to improve stability. In contrast to unilateral cases, patients with bilateral fractures frequently have longer hospital stays and more difficult rehabilitation despite proper therapy, highlighting the significance of obtaining secure fixation to enable early mobilization and enhance healing [14].
Due to the larger functional damage caused by the involvement of both lower limbs, rehabilitation for bilateral hip fractures is more difficult than for unilateral instances. In order to enhance recovery and restore function, early mobilization and improved physiotherapy are essential [12].
Early mobilization following hip fracture surgery is crucial for functional recovery because it has been demonstrated to be strongly linked to independent walking one year after the procedure. Additionally, it is associated with better gait recovery in the early postoperative phase. Although the precise mechanisms are still unknown, this impact might be linked to more opportunities for standing and walking activities, which aid in the regeneration of muscle strength [18].
In addition to improving functional recovery following hip fracture surgery, early mobilization is linked to a lower risk of long-term opioid medication up to a year after surgery [19]. Patients who were mobilized earlier, especially in the first 12 to 24 hours, showed a decreased risk of long-term opioid usage, indicating a dose-response connection in which higher results are achieved with earlier mobilization. The ability of early mobilization to counteract the detrimental physiological effects of immobilization, such as muscle weakness, bone deterioration, thromboembolic risk, and impaired systemic function—all of which may contribute to increased pain and the need for opioid analgesia—may account for this effect. Additionally, early mobilization may lessen the need for opioids by improving mental health, increasing functional independence, and lowering the frequency of unpleasant postoperative sequelae [20].
The simultaneous bilateral intertrochanteric fractures in our case emphasize how uncommon and complicated this injury pattern is, especially when high-energy trauma is not present. To guarantee stability and enable early deployment, the management necessitated meticulous surgical planning and the selection of suitable fixing techniques. Rehabilitation was more difficult because of the bilateral involvement, highlighting the significance of early physiotherapy to regain function. In line with previously documented mechanisms, this example also illustrates the influence of underlying bone quality, where osteoporosis may have contributed to the development of fractures even with minor damage.
4. Conclusion
Simultaneous bilateral intertrochanteric femur fractures are still a very uncommon and difficult clinical condition, especially in older patients following low-energy trauma. Even in the absence of high-energy mechanisms, their prevalence highlights the important influence of osteoporosis and reduced bone quality, which greatly enhance fracture risk.
Careful preoperative planning and a customized surgical strategy that takes the patient's overall health, bone quality, and fracture stability into account are necessary for the effective therapy of these injuries. Stable fixation is necessary for both fracture healing and early mobilization, which has been repeatedly linked to better functional outcomes, lower rates of complications, and less need for long-term opioid medication.
Additionally, the bilateral fractures create a great physiological and functional burden, which prolongs recovery and increases the difficulty of rehabilitation. To maximize perioperative care and improve recovery, this highlights the need for a multidisciplinary approach comprising orthopedic surgeons, anesthetists, physiotherapists, and geriatric specialists.
This case serves as more evidence that early detection, a suitable surgical approach, and postoperative rehabilitation are critical factors in excellent outcomes. It also emphasizes how crucial it is to treat underlying osteoporosis in order to enhance long-term patient prognosis and prevent further fractures.
Conflict of interest statement:
No conflict of interest exists.
Ethical approval:
Ethical approval was obtained from the Jordanian Royal medical services institutional Ethics Committee Amman-Jordan. Prior to study initiation. Written informed consent for publication, including all images, was obtained from the patient’s parents.
Statement of the location where the work was performed:
this study was performed in the Royal medical services king Hussein Medical hospital.
Patient consent:
Written informed consent was obtained from the patient for publication of this case report and accompanying images. Written consent is available for review by the Editor-in Chief of this journal on request.
Funding:
This research did not receive any fund.
References
- Viganò M, Pennestrì F, Listorti E, et al. Proximal hip fractures in 71,920 elderly patients: incidence, epidemiology, mortality and costs from a retrospective observational study. BMC Public Health 23 (2023): 1963.
- Walter N, Szymski D, Kurtz SM, et al. Epidemiology and treatment of proximal femoral fractures in the elderly US population. Scientific Reports 13 (2023): 12734.
- Walter N, Szymski D, Kurtz SM, et al. Complications and associated risk factors after surgical management of proximal femoral fractures. Bone and Joint Open 4 (2023): 801-807.
- Gillette DM, Cheng O, Wilson A, et al. Screening tool for identification of hip fractures in the prehospital setting. OTA International 4 (2021): e157.
- Rougereau G, Bourdier J-A, Langlais T, et al. Is there a femoral morphology at risk of a cervical or pertrochanteric fracture? Description and validation of the “Neck shaft ratio” and the “Intertrochanteric distal ratio” after analyzing a continuous cohort of 126 bilateral fractures of the proximal femur. Orthopaedics and Traumatology: Surgery and Research 110 (2024): 103874.
- Fischer H, Maleitzke T, Eder C, et al. Management of proximal femur fractures in the elderly: current concepts and treatment options. European Journal of Medical Research 26 (2021): 86.
- Che Y-J, Qian Z, Chen Q, et al. Effects of rehabilitation therapy based on exercise prescription on motor function and complications after hip fracture surgery in elderly patients. BMC Musculoskeletal Disorders 24 (2023): 817.
- Schroeder JD, Turner SP, Buck E. Hip fractures: diagnosis and management. American Family Physician 106 (2022): 675-683.
- Maffulli N, Aicale R. Proximal femoral fractures in the elderly: a few things to know, and some to forget. Medicina 58 (2022): 1314.
- Arshi A, Su L, Lee C, et al. Comparison of complication profiles for femoral neck, intertrochanteric, and subtrochanteric geriatric hip fractures. Archives of Orthopaedic and Trauma Surgery 143 (2023): 49-54.
- Chang S-M, Wang Z-H, Tian K-W, et al. A sophisticated fracture classification system of the proximal femur trochanteric region (AO/OTA-31A) based on 3D-CT images. Frontiers in Surgery 9 (2022): 919225.
- Zace P, Stephens A, Konstantinidis A, et al. Bilateral simultaneous proximal femoral fractures on dissimilar anatomical regions. Archive of Clinical Cases 12 (2025): 29.
- Aydın E, Dülgeroğlu TC, Metineren H. Bilateral simultaneous intertrochanteric fractures of femur without major trauma. International Medical Case Reports Journal 8 (2015): 137-139.
- Vaishya R, Agarwal AK, Nwagbara IC, et al. Simultaneous bilateral intertrochanteric fractures of the femur: a case report and review of the literature. Cureus 9 (2017).
- van der Zeeuw FT, Weeda VB, Vrouenraets BC. Simultaneous bilateral hip fractures following a simple fall in an elderly patient without predilecting comorbidities. Journal of Surgical Case Reports 2016 (2016): rjw050.
- Georgiadis GF, Chatzopoulos STD, Maniatis KA, et al. A rare case of an intertrochanteric hip fracture combined with an ipsilateral incomplete atypical femoral fracture treated with a long gamma intramedullary nail. Journal of Orthopaedic Case Reports 12 (2022): 65.
- Li X-P, Zhang P, Zhu S-W, et al. All-cause mortality risk in aged femoral intertrochanteric fracture patients. Journal of Orthopaedic Surgery and Research 16 (2021): 727.
- Nakamura K, Sasaki T, Kitagawa T, et al. Effect of early mobilization on gait recovery one year after hip fracture surgery: a single-center cohort study. Cureus 17 (2025).
- Agarwal N, MacLullich AM, Clement ND. Is the rate of early mobilization in hip fracture patients using Alfentanil better than standard opioid analgesia (REHAB)? A protocol for a prospective cohort study. Bone and Joint Open 6 (2025): 53-61.
- Tudorache YM, Andersen IT, Hjelholt TJ, et al. Association between early mobilization after hip fracture surgery and risk of long-term opioid therapy. European Geriatric Medicine 16 (2025): 921-931.



 Impact Factor:
* 5.3
Impact Factor:
* 5.3
 Acceptance Rate:
73.64%
Acceptance Rate:
73.64%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
