From Lung to Joint: Disseminated Tuberculous Arthritis Presenting as Multifocal Destructive Disease in a Patient with Poorly Controlled Diabetes
Abheek Raviprasad, Kevin Pierre, Kalyani Ballur, Diego A L Garcia*
Department of Radiology, University of Florida – Gainesville, FL, USA
*Corresponding Author: Diego A L Garcia, Department of Radiology, University of Florida – Gainesville, FL, USA.
Received: 10 April 2026; Accepted: 13 April 2026; Published: 20 April 2026
Article Information
Citation: Abheek Raviprasad, Kevin Pierre, Kalyani Ballur, Diego A L Garcia. From Lung to Joint: Disseminated Tuberculous Arthritis Presenting as Multifocal Destructive Disease in a Patient with Poorly Controlled Diabetes. Journal of Orthopedics and Sports Medicine. 8 (2026): 160-163.
View / Download Pdf Share at FacebookAbstract
Tuberculous arthritis is an uncommon form of musculoskeletal tuberculosis characterized by an indolent clinical course that frequently leads to delayed diagnosis and advanced joint destruction. We report the case of a 69-year-old male with poorly controlled type 2 diabetes mellitus complicated by retinopathy and nephropathy, who presented with progressive right shoulder pain. Magnetic resonance imaging demonstrated erosive inflammatory changes in the glenohumeral joint and incidentally revealed a cavitary lesion in the right upper lobe, highly suggestive of pulmonary tuberculosis. Subsequent clinical reassessment uncovered a history of chronic left hip pain preceding the shoulder symptoms. Imaging of the hip demonstrated advanced joint destruction. Histopathological and microbiological analyses confirmed Mycobacterium tuberculosis infection. This case highlights the importance of integrating imaging findings with clinical history and emphasizes how careful evaluation beyond the primary field of view may provide critical diagnostic clues. Tuberculosis should be considered in the differential diagnosis of chronic destructive arthritis, particularly in immunocompromised patients.
Keywords
Tuberculosis; Abscess; Cavitation; Neuropathic; Osteoarthritis; Arthropathy
Article Details
1. Introduction
Tuberculosis remains a major global health concern, with extrapulmonary manifestations accounting for approximately 15–20% of all active cases [1,2]. Musculoskeletal tuberculosis represents approximately 1–3% of total tuberculosis cases and about 10% of extrapulmonary disease [2,3]. The spine is the most affected site, followed by peripheral joints such as the hip and knee [3,4].
Tuberculous arthritis typically results from hematogenous dissemination of Mycobacterium tuberculosis, leading to chronic granulomatous synovitis that progressively destroys cartilage and subchondral bone [3,5]. Unlike acute septic arthritis, the disease evolves slowly, often over months or years, contributing to delayed diagnosis [6].
The hip joint is one of the most frequently involved peripheral joints, whereas shoulder involvement is less common [4,7]. Multifocal joint involvement is relatively rare and may complicate clinical recognition [8].
Risk factors for extrapulmonary tuberculosis include immunosuppression and chronic systemic diseases such as diabetes mellitus, which impairs host immune response and increases susceptibility to infection [9].
We present a case of disseminated tuberculous arthritis involving the hip and shoulder in a patient with poorly controlled diabetes mellitus, emphasizing the role of imaging in diagnosis and the importance of recognizing patterns of hematogenous spread.
2. Case Presentation
A 69-year-old male with a history of poorly controlled type 2 diabetes mellitus complicated by diabetic retinopathy and nephropathy presented with progressive right shoulder pain over three months. The pain had an insidious onset and progressively worsened, becoming associated with stiffness and limitation of motion.
The patient denied recent trauma. Constitutional symptoms such as fever, night sweats, or weight loss were absent or minimal. Physical examination demonstrated moderate restriction in the range of motion of the right shoulder without overt inflammatory signs. Laboratory evaluation revealed mildly elevated inflammatory markers with normal leukocyte count.
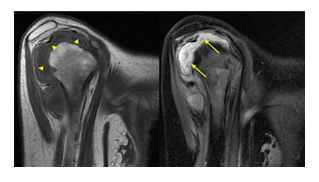
Magnetic resonance imaging (MRI) of the right shoulder demonstrated synovial thickening, joint effusion, and multiple erosions involving the humeral head and glenoid, associated with bone marrow edema. These findings favored chronic infectious or inflammatory arthropathy rather than an acute pyogenic process [10,11].
Importantly, the imaging field included the ipsilateral lung apex, where an incidental cavitary lesion with irregular thickened walls was identified. This finding raised strong suspicion for active pulmonary tuberculosis.
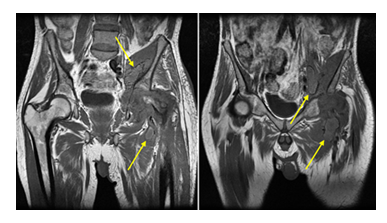
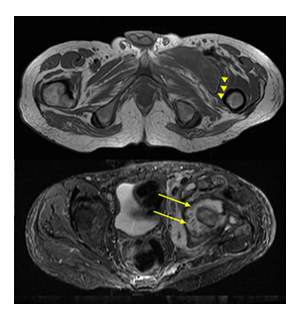
Following this finding, further history revealed chronic left hip pain preceding the shoulder symptoms by approximately one year. Imaging of the hip demonstrated severe joint space narrowing, extensive osseous erosions, partial collapse of the femoral head, and marked periarticular osteopenia, consistent with advanced chronic destructive arthritis [4,12].
Given the combination of indolent symptoms, multifocal joint involvement, and cavitary pulmonary lesion, disseminated tuberculosis was strongly suspected. Joint aspiration and biopsy revealed granulomatous inflammation with caseating necrosis, and microbiological analysis confirmed Mycobacterium tuberculosis infection.
3. Imaging Findings
MRI of the right shoulder demonstrated synovial hypertrophy, joint effusion, and osseous erosions involving the humeral head and glenoid, findings consistent with chronic infectious arthritis [10,11].
The incidental cavitary lesion identified in the right upper lobe is a classic manifestation of post-primary pulmonary tuberculosis and is associated with a high bacillary burden [13].
Imaging of the left hip demonstrated advanced destructive changes, including joint space narrowing, extensive erosions, partial femoral head collapse, and periarticular osteopenia, corresponding to the classic Phemister triad [4,12].
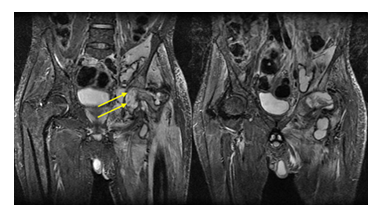
MRI also demonstrated the penumbra sign, representing granulation tissue lining an abscess cavity, which is highly suggestive of subacute or chronic infection and can aid in differentiating tuberculosis from other etiologies [10].
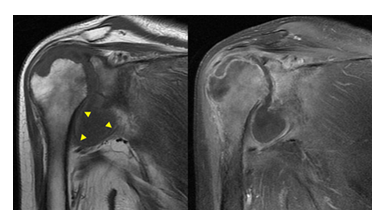
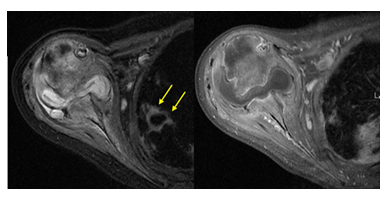
Figure 1: Coronal T1-weighted images demonstrating severe destruction of the femoral head with periarticular collections in the left hip and iliacus muscle, showing a similar penumbra-like signal (arrows) at the periphery of the collection. This sign is due to paramagnetic free radicals produced by activated macrophages and is considered highly specific (99%) for abscess.
4. Discussion
Tuberculous arthritis results from hematogenous dissemination of Mycobacterium tuberculosis, most commonly from a pulmonary source [3,5]. Once the synovium is seeded, chronic granulomatous inflammation leads to progressive cartilage destruction and osseous erosion.
A key teaching point is the indolent nature of osteoarticular tuberculosis. Symptoms are often mild and nonspecific, contributing to delayed diagnosis and advanced joint destruction at presentation [6].
In this case, the likely progression from pulmonary infection to hip involvement and subsequently to the shoulder illustrates the potential for systemic dissemination and multifocal disease.
Characteristic imaging findings include the Phemister triad and the penumbra sign, both of which support the diagnosis of chronic granulomatous infection [4,10,12].
An important radiologic teaching point highlighted by this case is the need for systematic evaluation of all structures within the imaging field. The incidental detection of a cavitary pulmonary lesion on shoulder MRI was pivotal in establishing the diagnosis. Failure to recognize such findings may contribute to diagnostic delay.
Tuberculosis should be considered in the differential diagnosis of chronic monoarthritis or oligoarthritis, particularly in patients with risk factors such as diabetes mellitus or immunosuppression [9,14].
5. Conclusion
This case emphasizes the indolent and destructive nature of tuberculous arthritis and highlights the importance of maintaining a high index of suspicion in patients presenting with chronic joint symptoms. Careful evaluation of imaging beyond the primary region of interest may reveal critical findings that significantly impact diagnosis and management.
References
- Pigrau-Serrallach C, Rodríguez-Pardo D. Bone and joint tuberculosis. Eur Spine J 22(2013): S556-S566.
- Golden MP, Vikram HR. Extrapulmonary tuberculosis: an overview. Am Fam Physician 72 (2005):1761-1768.
- Vanhoenacker FM, Sanghvi DA, De Backer AI. Imaging features of extra-axial musculoskeletal tuberculosis. Indian J Radiol Imaging 19 (2009): 176-186.
- Agarwal A, Qureshi NA, Khan SA, et al. Skeletal tuberculosis: evolving imaging patterns. Skeletal Radiol 49 (2020): 1835-1851.
- Tuli SM. Tuberculosis of the Skeletal System. 4th ed. Jaypee Brothers (2010).
- Jain AK, Dhammi IK. Tuberculosis of the skeletal system. Indian J Orthop 41 (2007): 198-205.
- Rasool MN, Govender S. Tuberculosis of the shoulder joint. J Bone Joint Surg Br 71 (1989): 753-756.
- Martini M, Adjrad A. Tuberculous arthritis. Orthop Clin North Am 15 (1984): 639-654.
- Lee JY. Diagnosis and treatment of extrapulmonary tuberculosis. Tuberc Respir Dis 78 (2015):47-55.
- Hong SH, Kim SM, Ahn JM, et al. Tuberculous versus pyogenic arthritis: MR imaging evaluation. Radiology 218 (2001): 848-853.
- Sawlani V, Chandra T, Mishra RN, et al. MRI features of tuberculosis of peripheral joints. Clin Radiol 58 (2003): 755-762.
- Griffith JF, Kumta SM, Leung PC, et al. Imaging of musculoskeletal tuberculosis. Clin Orthop Relat Res 398 (2002): 32-39.
- World Health Organization. Global Tuberculosis Report 2023. Geneva: WHO (2023).
- Berbari EF, Kanj SS, Kowalski TJ, et al. Infectious arthritis: epidemiology, diagnosis, and treatment. Clin Infect Dis 61 (2015): e1-e25.


 Impact Factor:
* 5.3
Impact Factor:
* 5.3
 Acceptance Rate:
73.64%
Acceptance Rate:
73.64%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
