Incidental Distal Femoral Melorheostosis in a Patient with Medial Knee Pain Due to Medial Meniscus Posterior Root Tear
Sylvia Arce, Kalyani Ballur, Diego A L Garcia*
Department of Radiology, University of Florida, Gainesville, Florida, USA
*Corresponding Author: Diego A L Garcia, Department of Radiology, University of Florida – Gainesville, FL, USA
Received: 23 April 2026; Accepted: 27 April 2026; Published: 04 May 2026
Article Information
Citation: Sylvia Arce, Kalyani Ballur, Diego A L Garcia. Incidental Distal Femoral Melorheostosis in a Patient with Medial Knee Pain Due to Medial Meniscus Posterior Root Tear Journal of Orthopedics and Sports Medicine 8 (2026): 170-173.
View / Download Pdf Share at FacebookAbstract
Melorheostosis is a rare benign sclerosing bone dysplasia characterized by eccentric cortical hyperostosis, classically described as a “dripping candle wax” appearance on radiographs. Although some patients are symptomatic, many lesions remain clinically silent and are discovered incidentally during imaging performed for unrelated complaints. Accurate recognition is important because its striking appearance may mimic aggressive osseous pathology and prompt unnecessary investigation. We report a 70-year-old man presenting with medial knee pain. Radiographs and magnetic resonance imaging (MRI) demonstrated classic melorheostosis involving the lateral distal femur. However, MRI also revealed a posterior root tear of the medial meniscus with meniscal extrusion and reactive inflammatory change involving the medial supporting structures of the knee, concordant with the patient’s symptoms. The distal femoral lesion showed benign chronic imaging features without marrow edema, cortical destruction, or soft-tissue mass. This case highlights the importance of distinguishing incidental imaging abnormalities from the true pain generator and recognizing characteristic features of melorheostosis to avoid unnecessary biopsy, oncologic referral, and patient anxiety.
Keywords
Melorheostosis; Meniscus Root Tear; Knee Pain; Incidental Lesion; Musculoskeletal MRI
Article Details
1. Introduction
Melorheostosis is an uncommon nonhereditary sclerosing mesenchymal dysplasia first described by André Léri and J. Joanny in 1922. The disorder is characterized by irregular cortical and endosteal hyperostosis, often distributed longitudinally along one limb or contiguous skeletal segment. The appendicular skeleton, particularly the lower extremities, is most frequently affected. Clinical manifestations are heterogeneous and range from asymptomatic incidental lesions to chronic pain, stiffness, contractures, deformity, and functional limitation. Radiographs are frequently diagnostic when the classic flowing cortical hyperostosis pattern is present. However, unfamiliar readers may confuse melorheostosis with parosteal neoplasm, metastatic disease, chronic osteomyelitis, or other sclerosing bone lesions. We report an elderly patient undergoing evaluation for medial knee pain in whom imaging demonstrated incidental distal femoral melorheostosis, while MRI identified the actual symptomatic abnormality: posterior root tear of the medial meniscus with extrusion-related medial compartment inflammation.
2. Case Presentation
A 70-year-old man presented with chronic right knee pain localized to the medial joint line. Symptoms were mechanical in nature, worsened by prolonged walking, stair climbing, squatting, and twisting maneuvers. He denied recent trauma, fever, unexplained weight loss, prior malignancy, or previous knee surgery. Physical examination demonstrated focal tenderness along the medial femorotibial joint line with pain during meniscal provocative maneuvers. No palpable mass, swelling, or focal tenderness was present over the lateral distal femur. Conventional radiographs of the knee demonstrated mild medial compartment degenerative change and an elongated dense cortical hyperostotic lesion along the lateral aspect of the distal femoral metaphysis extending into the supracondylar region. The lesion was contiguous with cortex and demonstrated classic flowing hyperostosis consistent with the “dripping candle wax” morphology of melorheostosis. No cortical destruction, aggressive periosteal reaction, pathologic fracture, or associated soft-tissue mass was identified.
MRI obtained for internal derangement demonstrated a posterior root tear of the medial meniscus with associated meniscal extrusion. Reactive edema and inflammatory change involved the adjacent medial capsuloligamentous supporting structures. Mild chondral degeneration of the medial compartment was also present. These findings were concordant with the patient’s symptoms. The distal femoral lesion corresponded to marked cortical thickening with uniformly low signal intensity on T1- and T2-weighted sequences, without marrow edema, cortical breakthrough, surrounding soft-tissue abnormality, or other aggressive imaging feature. Given the concordant medial compartment pathology and the anatomically separate asymptomatic lateral femoral lesion, the patient’s pain was attributed to medial meniscus posterior root insufficiency rather than melorheostosis. Conservative management was directed toward the symptomatic knee pathology.
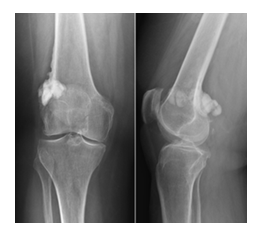
Figure 1: Anteroposterior (AP) and lateral radiographs of the right knee demonstrate the classic “dripping candle wax” appearance of melorheostosis, characterized by flowing cortical sclerosis along the lateral femoral cortex involving the lateral supracondylar distal femur. The osseous abnormality is best appreciated on the AP view. Associated extraosseous/soft-tissue extension of the hyperostotic process is better visualized on the lateral view.
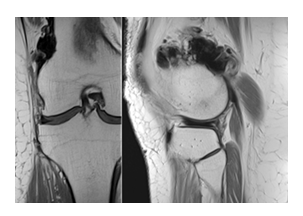
Figure 2: Coronal T1-weighted and sagittal proton density (PD) MR images demonstrate the same lesion seen on radiographs, involving the lateral distal femur with characteristic flowing cortical hyperostosis. The sclerotic components show diffusely low signal intensity on both sequences, consistent with densely mineralized bone.
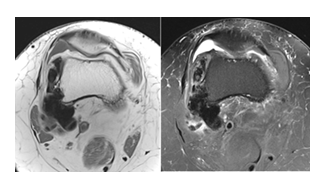
Figure 3: Axial T1-weighted and axial T2 fat-suppressed MR images demonstrate juxtacortical sclerotic ossified tissue extending into the lateral and posterior peri-femoral soft tissues. These areas show marked low signal intensity on all evaluated sequences, consistent with densely mineralized melorheostotic involvement.
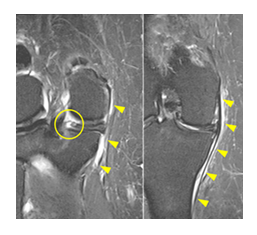
Figure 4: Coronal T2-weighted fat-suppressed MR images demonstrate a posterior root tear of the medial meniscus (circle) with mild meniscal diastasis resulting in meniscal extrusion. Associated reactive inflammatory edema (arrowheads) is present within the medial supporting structures of the knee, compatible with mechanically mediated stress-related change.
3. Discussion
This case illustrates a fundamental principle in musculoskeletal imaging: not every imaging abnormality is the pain generator. Incidental osseous lesions may coexist with common symptomatic knee disorders, particularly in older adults undergoing imaging for degenerative complaints. Accurate clinicoradiologic correlation remains essential. Melorheostosis is classically recognized radiographically by eccentric cortical hyperostosis extending longitudinally along the cortex, producing the well-known “dripping candle wax” appearance. When classic morphology is present, radiographs are often sufficient for diagnosis. MRI may be less specific for lesion characterization but is valuable for confirming the absence of aggressive features and simultaneously evaluating alternative symptomatic pathology, as in this case.
Several imaging features supported a benign incidental melorheostotic lesion in our patient:
- • dense mature cortical sclerosis
- • longitudinal flowing hyperostosis
- • absence of cortical destruction
- • absence of marrow edema
- • no aggressive periosteal reaction
- • no soft-tissue mass
- • no local tenderness corresponding to lesion location.
In contrast, the patient’s symptoms were explained by posterior root failure of the medial meniscus. The posterior root is essential for maintaining hoop stress transmission. Root tears biomechanically resemble subtotal meniscectomy, allowing meniscal extrusion and increased focal load across the medial compartment. Resultant capsular traction, synovial irritation, and inflammatory reaction of adjacent supporting structures may generate substantial pain even in the absence of advanced osteoarthritis. Recognition of this distinction has practical implications. Misattribution of symptoms to the dramatic distal femoral lesion could have led to unnecessary oncologic referral, serial surveillance imaging, biopsy, or patient distress, while delaying treatment of the true symptomatic disorder. Recent molecular studies have identified somatic activating mutations involving the MAPK pathway, particularly MAP2K1, in subsets of patients with melorheostosis, supporting a mosaic developmental mechanism. Management remains symptom based. Observation is appropriate for asymptomatic incidental lesions, whereas painful or function-limiting disease may require analgesia, physiotherapy, or selected surgical treatment.
4. Conclusion
Melorheostosis may be incidentally encountered during imaging performed for common knee complaints. In this patient, classic lateral distal femoral melorheostosis was anatomically distinct from the true pain generator: medial meniscus posterior root tear with extrusion-related inflammatory change. Recognition of characteristic imaging findings, together with careful symptom correlation, enabled confident diagnosis and avoidance of unnecessary invasive investigation. Familiarity with this rare benign entity remains valuable for radiologists interpreting routine knee studies.
Learning Points
- Melorheostosis may remain asymptomatic into late adulthood and be discovered incidentally.
- Not all striking imaging abnormalities explain knee pain.
- Radiographs are often diagnostic when classic flowing cortical hyperostosis is present.
- MRI is valuable for excluding aggressive features and identifying the true symptomatic pathology.
- Medial meniscus posterior root tears may cause extrusion-related inflammatory medial knee pain.
- Correct recognition can prevent unnecessary biopsy, referral, cost, and anxiety.
References
- Léri A, Joanny J. Une affection non décrite des os: hyperostose en coulée sur toute la longueur d’un membre ou melorhéostose. Bull Mem Soc Med Hop Paris 46 (1922): 1141-1145.
- Campbell CJ, Papademetriou T, Bonfiglio M, et al. A report of the clinical, roentgenographic, and pathological findings in fourteen cases. J Bone Joint Surg Am 50 (1968): 1281-1304.
- Freyschmidt J. Melorheostosis: a review of 23 cases. Eur Radio 11 (2001): 474-479.
- Murray RO, McCredie J. Melorheostosis and the sclerotomes. Lancet 2 (1979): 1360-1362.
- Judkiewicz AM, Murphey MD, Resnik CS, et al. Advanced imaging of melorheostosis with emphasis on MRI and CT. Skeletal Radiol 30 (2001): 447-453.
- Kang H, Jha S, Deng Z, et al. Somatic activating mutations in MAP2K1 cause melorheostosis. Nat Commun 9 (2018): 1390.
- LaPrade RF, Ho CP, James E, et al. Diagnostic accuracy of 3.0 Tesla MRI for the detection of posterior root pathology of the lateral and medial meniscus. Knee Surg Sports Traumatol Arthrosc 23 (2015): 152-157.
- Bhatia S, LaPrade CM, Ellman MB, et al. Meniscal root tears: significance, diagnosis, and treatment. Am J Sports Med 42 (2014): 3016-3030.
- Allaire R, Muriuki M, Gilbertson L, et al. Biomechanical consequences of a tear of the posterior root of the medial meniscus. Similar to total meniscectomy. J Bone Joint Surg Am 90 (2008): 1922-1931.
- Krych AJ, Reardon PJ, Johnson NR, et al. Nonoperative management of medial meniscus posterior horn root tears: an observational study. Knee Surg Sports Traumatol Arthrosc 25 (2017): 383-389.
- De Smet AA, Mukherjee R. Clinical, MRI, and arthroscopic findings associated with meniscal root tears. AJR Am J Roentgenol 191 (2008): 80-85.
- Bernard CD, Kennedy NI, Tagliero AJ, et al. Medial meniscus posterior root tear treatment: a matched cohort comparison of nonoperative management, partial meniscectomy, and repair. Am J Sports Med 48 (2020): 128-132.


 Impact Factor:
* 5.3
Impact Factor:
* 5.3
 Acceptance Rate:
73.64%
Acceptance Rate:
73.64%
 Time to first decision: 10.4 days
Time to first decision: 10.4 days
 Time from article received to acceptance:
2-3 weeks
Time from article received to acceptance:
2-3 weeks
